Treating Clubfoot
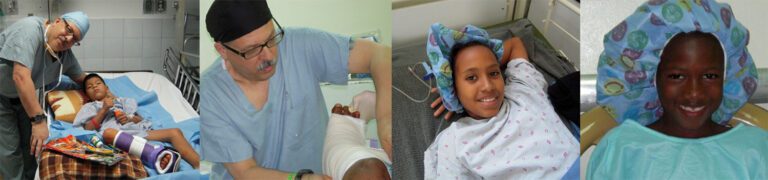
Treating clubfoot and supporting families along the way The job of the pediatric orthotist is to provide customized AFO boots that will need adjustments and replacements as the child grows. An experienced orthotist will educate the parents about daily care and what devices will be used, and how they can be customized. Consultation and direction…